Getting enough calcium and vitamin D is crucial for building children’s bones and keeping them strong and healthy as we age. Calcium is also necessary for helping blood clot and teeth. Each day we lose calcium through our sweat, urine, skin, nails and hair but out bodies cannot make new calcium. It is therefore essential to absorb calcium from the food we eat. When our diets fall short of calcium, it is taken from our bones.
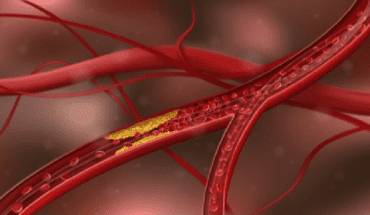
Foods such as dairy, nuts, leafy greens and fish are rich in calcium and help to keep your bones strong and protect them against osteoporosis. Calcium and vitamin D supplements can be useful for people with deficiencies, or who are allergic to dairy produce, or nuts and dislike green vegetables. Calcium and vitamin D supplements, which usually come in the forms of tablets, are widely used and have been generally viewed as relatively safe, but some researchers have previously raised concerns over potential links with cardiovascular disease.
In contrast, our researchers at the University of Southampton found no association between the use of calcium or vitamin D supplementation and cardiovascular events such as heart attacks. The study was based on the UK Biobank, a study involving 502, 664 men and women aged 40-69 years.
In contrast, our researchers found no association between the use of calcium or vitamin D supplementation and cardiovascular events such as heart attacks. The study was based on the UK Biobank, a study involving 502, 664 men and women aged 40-69 years.
In the new study, which was led by myself and recently published in the Journal of Bone and Mineral Research, investigators from the Medical Research Council Lifecourse Epidemiology Unit (MRC LEU), University of Southampton used the internationally unique UK Biobank cohort, to explore relationships between the use of calcium and/or vitamin D supplementation and the risk of cardiovascular events such as heart attacks.
The analysis accounted for a wide range of other potential influences, and did not detect any statistically significant associations between use of the supplements and events such as heart attacks, hospital admission for angina, or related deaths.
The results are the first in such a large cohort of both men and women, with previous studies focused mainly on women. They are also the first to investigate the issue in such a large cohort in which both the exposures and the outcomes have been defined and sampled in a uniform fashion, with information on cardiovascular outcomes and deaths obtained from linkage to Hospital Episode Statistics and ONS Death Registry data.
Calcium and vitamin D supplements are widely used in the population, and are particularly appropriate for those individuals at risk of deficiency in either nutrient. In this situation there is good evidence that they provide a modest reduction in fracture risk, although do not replace medications specifically licensed for the treatment of osteoporosis.
Whilst our current findings can never be absolutely definitive compared with those from a comprehensive randomised controlled trial, it is unlikely to be possible to undertake this sort of trial in practice, and our results provide reassuring findings with regard to cardiovascular outcomes, at least within the age range studied. Further study will be needed as this population ages, to examine whether the lack of association persists into older age.
- Calcium and Vitamin D supplements don’t increase risk of CVD - 26th February 2018
- Risk of breaking a bone depends on where you live - 6th April 2016