Food plays an integral part in our lives and we all spend time thinking about what we have eaten, or what we are going to eat. Sometimes we may try to eat more healthily, try a diet, have cravings, eat more than usual or lose our appetite. Changing your eating habits every now and again is normal. This article will help you recognise early signs and broach difficult conversations should you feel that there is something seriously wrong.
Sometimes food and eating becomes an obsession and feels like it’s an overwhelming part of life. This is when it becomes a problem.
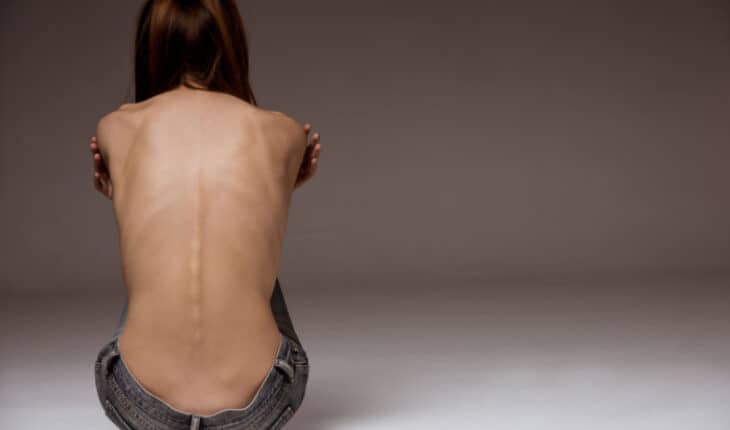
When someone has an eating disorder, they will often eat too much or too little, or binge and make themselves sick, or use laxatives. They can become obsessed with their body weight and appearance and what they see when they look in the mirror can be very different to the reality.
It is often believed that if someone has an eating problem they will always noticeably appear under or overweight – this is not the case! Anyone, regardless of their weight, age or gender can be seriously affected by an eating disorder.
Eating problems vs Eating disorders
After someone develops eating problems it can go on to become an eating disorder.
- An eating disorder is a medical diagnosis based on eating patterns, medical tests, weight, blood and body mass index (BMI).
- An eating problem is a difficult relationship with food. This can be just as hard to live with as a diagnosed eating disorder.
Eating problems tend not to be just about food. They can be a way of coping with difficult things and painful feelings, which the person may find hard to express, face or resolve. Therefore, focusing on food can be a way of disguising these problems, sometimes the individual themselves may not realise this is the case.
Lots of people have different eating habits. You might be known as a fussy eater, eat loads one day, less another day, try diets and want to eat more or less healthily. But none of these mean you have an eating problem.
However, if you focus on controlling what or how much you eat, or if you have urges to eat and then make yourself sick (bulimia), or try using laxatives afterwards, these are signs you could have a problem.
How common are eating disorders?
Eating problems are common and they affect people with any body shape or lifestyle. Between 1.25 and 3.4 million people in the UK are affected by an eating disorder. Around 25% of those affected by an eating disorder are male. Most eating disorders develop during adolescence, although there are cases of eating disorders developing in children as young as 6 and in adults in their 70’s.
All kinds of things can lead to eating problems or disorders. Sometimes people develop an eating problem to try and control something in their life when they are feeling worried, stressed or feeling out of control. Sometimes social media and media portrayal can lead people to feel they have to look a certain way, or be a certain weight which may not be healthy.
Often what someone sees when they look in the mirror is totally different to what they really look like.
Signs someone could have an eating problem
Here are some indicators that someone could be experiencing an eating problem:
If they are regularly:
- Not wanting to eat or eating when not hungry
- Obsessing about their body (e.g. being too fat, need a 6 pack or more muscles)
- Eating only certain types of things or following fad diets
- Afraid of gaining weight
- Their appearance may change, becoming noticeably fatter or thinner
- Making themselves sick
- May eat very slowly and cut their food up very small or eat a lot of food very fast
- No longer enjoying eating socially or leaving the table quickly (to be sick or hide food or visit the bathroom)
- Obsessing about buying or cooking food for others
- Being secretive about eating and preoccupied with food
- Being self-conscious about eating in front of others
- Struggling to concentrate and feel tired a lot
- Become depressed and anxious
- Appear unwell and sluggish
- Lose their spontaneity and no longer want to travel or to go anywhere new
- Frequently compare their body weight or image with others.
Many people manage to hide their eating problems – sometimes they can successfully manage this for a very long time.
A person’s weight on its own does not determine whether they have a problem.
Being able to control how much they eat often gives a feeling of order but can lead to more serious issues.
Some eating problems become serious mental health conditions that need professional intervention to diagnose and treat.
In serious cases and without the right kind of support and treatment, they can even result in death, which is why it is so important to get help as soon as possible.
Recovering from an eating disorder can be a long process, but with the right help a full recovery is possible.
What to do if you think you have an eating problem
Speak to your GP for advice. Sometimes learning to eat normally again can be hard work, so your doctor can help you get the support you need. They might suggest talking therapies that involve the whole family. They will help you deal with the issues that may have triggered the eating problem.
The doctor may also want to measure your weight to assess your BMI (Body Mass Index) –many people are nervous about this; however it is vital to remember that they don’t want to judge, they need this information to help.
Avoid apps, accounts or websites that contribute to your negative body image and your relationship with eating.
Eating problems and links with other mental health problems
Often people with eating problems also have other mental health problems, such as depression, anxiety or obsessive-compulsive disorders. An anxiety disorder called body dysmorphic disorder results in extreme anxiety around body image and often leads to eating disorders.
For some people, eating problems are linked to self-harm – and this may lead them to hurt themselves in other ways too. Sometimes someone can develop a phobia around certain foods, that can become overwhelming and lead to eating problems and for others it could be related to self-esteem. Some people don’t know how or why it has happened and do not realise they have a problem.
How to approach someone with an eating disorder – The CARES approach
Check for life-threatening problems. Calmly approach, reassure, assess & assist.
Before approaching the person, it is helpful to take time to familiarise yourself with the symptoms and treatments of eating disorders so you are have a greater understanding about what you suspect they might be experiencing. This will help you approach more sensitively and with greater empathy.
Choose an appropriate, safe, comfortable space where you are unlikely to be disturbed.
Don’t approach them to talk about this at mealtimes, in an eating environment, or when other people are around.
Actively Listen without judgment
Ask open questions and explain why you are worried in an open and honest manner. Ask how they are feeling and if you can help?
Try not to focus on food or bodyweight.
Incredibly important to listen openly and without judgement.
Recommend sources of immediate help – be particularly aware of signs of crisis
See if there is anything practical you can do to alleviate some of their immediate stress?
Encourage to seek professional help
In addition, explain that you think their symptoms indicate a need to seek professional help
The person may react positively to having a helping hand and feel a sense of relief that someone has noticed there is a problem.
Alternatively (and more likely), the person may deny there is a problem and be reluctant to seek professional help.
Try not to reason with them, or be angry if your help is dismissed, let them know you will be there for them if they need you.
Reassure the person that they can be helped and with the right support, could feel a lot better.
If they feel comfortable getting help, the best person for them to see in the first instance is their GP. Also, ideally they would visit their GP with a close friend or relative.
Treatments
There are a variety of online self-help therapies that GPs can refer to, that many people find helpful.
In addition, GPs can refer someone to talking treatments such as CBT and help the person to access support networks.
- Cognitive behavioural therapy for eating disorders (CBT–ED). This is an adapted form of CBT specifically for treatment of eating disorders, including anorexia. There are alternative forms of CBT for bulimia nervosa (CBT-BN) and binge eating disorder (CBT-BED).
- For anorexia, someone should be offered up to 40 sessions, with twice weekly sessions in the first two or three weeks.
- Someone suffering from bulimia should be offered at least 20 sessions, and may be offered twice weekly sessions at first.
- For binge eating disorder someone should be offered group CBT sessions at first.
- Family therapy. This means working through issues as a family with the support of a therapist and exploring family dynamics or situations that might have prompted the feelings underlying an eating disorder. Overall, it can be extremely helpful for the whole family to understand the best way to support and help them recover.
- The frontline NICE accredited treatment offered by the NHS for adolescents with anorexia is Family Based Treatment. FBT does not look at family dynamics, which may be irrelevant to the eating disorder. Instead it supports parents to take control of food and does not introduce any form of talking therapy until the patient’s brain has recovered from malnutrition. In most cases a starving individual’s brain is not capable of engaging in talking therapy so the focus is on re-feeding. Many of the eating disorder behaviours and beliefs disappear or reduce simply with nourishment.
- It is really important to understand that people can recover fully from eating disorders.
Suggest possible self-help and other support options for better mental health
Useful resources for Eating Disorders:
Anorexia and Bulimia Care (ABC)
03000 11 12 13
anorexiabulimiacare.org.uk
Advice and support for anyone affected by eating problems.
Association for Family Therapy and Systemic Practice
aft.org.uk
Information about family therapy, including a directory of therapists.
B-EAT
Beat is the UK’s leading charity supporting anyone affected by eating disorders.
0808 801 0711 (youthline)
0808 801 0811 (studentline)
beateatingdisorders.co.uk
Under 18s helpline, webchat and online support groups for people with eating disorders, such as anorexia and bulimia.
British Association for Behavioural and Cognitive Psychotherapies (BABCP)
babcp.com
Information about cognitive behavioural therapy and related treatments, including details of accredited therapists.
British Association for Counselling and Psychotherapy (BACP)
bacp.co.uk
Professional body for talking therapy and counselling. Provides information and a list of accredited therapists.
Men Get Eating Disorders Too
Support and advice for men with eating disorders
National Centre for Eating Disorders
eating-disorders.org.uk
Everything you need to know about eating disorder treatments, information and professional training.
NICE
nice.org.uk
Produces guidelines on best practice in healthcare.
Overeaters Anonymous Great Britain
oagb.org.uk
Local support groups for people with eating problems.
Papyrus HOPELINEUK
0800 068 41 41
07786 209697 (text)
papyrus-uk.org
Confidential support for under-35s at risk of suicide and others who are concerned about them.
Samaritans
116 123 (freephone)
[email protected]
Freepost RSRB-KKBY-CYJK
PO Box 90 90
Stirling FK8 2SA
samaritans.org
Open 24/7 for anyone who needs to talk. You can visit some branches in person.
SEED
seedeatingdisorders.org.uk
A group of ordinary people with first-hand experience of eating disorders.
Student Minds
studentminds.org.uk
Mental health charity that supports students.
Tommy’s
tommys.org
Information and support for people affected by stillbirth, miscarriage and premature birth.
YoungMinds
0808 802 5544 (parents helpline)
85258 (crisis messenger service, text YM)
youngminds.org.uk
Committed to improving the mental health of babies, children and young people, including support for parents and carers.
- What is a seizure? - 13th March 2025
- Febrile Convulsions and Seizures in Children - 13th March 2025
- Why women are less likely to receive CPR or survive cardiac arrest - 6th March 2025