“What to expect when going for cervical screening” is part of the ‘How it works now‘ series from Jo’s Cervical Cancer Trust, aimed at helping women to navigate how the healthcare system works during the pandemic.
One common question we are asked is what to expect when going for cervical screening at the moment. This is something that we can’t provide you with an exact answer for, as it will be different in different areas.
Each practice is putting measures in place to make attending for you, other patients and those working in the practice, safe. There are lots of factors including the size of the practice and the layout, the number of patients and the equipment and resources they have.
The team at Jo’s Cervical Cancer have spoken with Jenny, Debra and Tracey, who are all nurses, about what their GP practice is doing, to give you an idea of the measures that you could see and help you to prepare any questions.
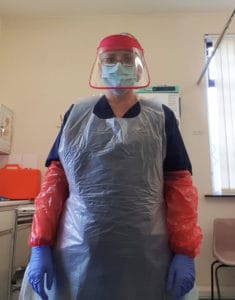
Don’t worry if some of measures below aren’t in place at your practice. There are lots of measures that can be implemented to keep you safe. This includes use of personal protective equipment (PPE), social distancing and frequent cleaning.
Your GP practice should let you know what measures they have in place before your appointment, but you can always call them and ask them what to expect.
Don’t forget that you should only visit your GP in person if they tell you to.
Jenny:
“We phone everyone visiting the practice beforehand to check they do not have any coronavirus symptoms. We also do say when we phone them before the appointment that things are different now and I would say that the majority are happy to know that we are trying to keep them safe and seem to accept what is happening. Patients are asked to come alone and we don’t allow people in the waiting room at the moment, instead patients come to a side entrance and we collect them when we are ready. We try to be on time and ask patients to only arrive at the time of their appointment, but if we are delayed or the patient is early then we have a bell attached to a speaker phone, so reception can let us know they have arrived.”
Debra:
“All patients are telephone triaged, this means that those at higher risk of coronavirus or with potential symptoms can be kept away from other patients. We also ask all patients to fill out a short survey asking about potential coronavirus symptoms ahead of their visit.
We know that it can feel a bit strange for patients so we always ring ahead of appointments to explain all the safety measures they can expect to see – this usually helps to put people at ease. Patients come to the staff entrance as that’s the nearest door to the room used for screening. They have to wait outside until their appointment time when I’ll collect them and take them straight into the consultation room. We arrange appointments so that patients don’t see anyone else while at the practice and it’s always the same person who escorts you out too.”
Tracey:
A sign saying ‘green zone’ in the car park of a GP surgery.“We’re a large practice with 9 nurses in the team! At the moment, we’re holding cervical screening clinics on Monday, Tuesday and Wednesday mornings. Having specific clinics on specific days means we can take any additional measures we might need to keep patients safe. Screening takes place in the ‘green zone’ in the practice – we have red, amber and green zones – allowing us to keep patients at highest risk such as those shielding or with symptoms away from other.”
“We don’t have receptionists anymore, instead a healthcare assistant greets patients and asks them a few questions to see if they have symptoms and so a temperature check. We then take them straight to the examination room, so they don’t have to wait in a waiting room. This system helps us make sure we don’t have people arriving or leaving at the same time. The practice is actually really quiet so if you are worried about bumping other people, now might be the time to go!
Jenny:
“We don’t ask patients to wear masks or gloves. However, we have a table near to the entrance door, which has gloves, masks and hand sanitiser on it which patients can use. A lot of patients are already coming along with their own masks and also hand sanitiser. In our rooms we have hand washing facilities and I offer this at the time of their smear and after.”
Debra:
“We provide everyone coming into the practice with a mask and gloves. I take the gloves off I let them in with, wash my hands and put on fresh gloves and plastic sleeves ahead of the test, so at no point will there be any skin touching.”
Tracey:
“The nurses all wear masks, eye protection, scrubs, an apron and gloves. This can be quite daunting for patients, especially if it’s the first time they have seen anyone in full protective clothing, or are feeling worried but don’t worry we’re just the same underneath and can carry out the test just as well. The test itself is exactly the same, it’s only us who might look a bit different with our PPE on! We encourage patients to wear masks and provide hand sanitiser too.
At a smaller practice down the road, they wear aprons and gloves as they only take low risk patients at the moment and send those at greater risk to practices such as ours, where we have appropriate zones.”
Debra:
“We always kept the practice clean, however we’ve increased the amount of cleaning carried out including extending appointments to 30 minutes so we can do even more cleaning between patients.”
Tracey:
“We always keep the practice clean but are conducting additional cleaning between patients at the moment. We are still seeing lots of patients through video or phone calls and some patients are seen in their cars, do remember that if we do decide to bring people in it’s because it’s safe.
Find more information about cervical screening and coronavirus on the Jo’s Trust Cervical Cancer information hub.
- Covid-19 cervical screening – what to expect? - 17th June 2020