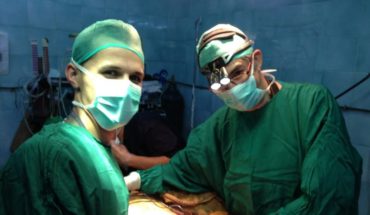
After a decade of volunteering in war zones, Elma knows all too well how important education is. When she heard we were looking to deepen our impact by upskilling anaesthetists in conflict zones, Elma jumped at the chance to get involved.
“I’m interested in building up local workforces, making communities in conflict more sustainable. It’s about the longevity of the impact you want to have in a place.
The biggest gift you can give to a healthcare worker in a conflict zone is self-sufficiency – the dignity to be able to do everything themselves. It’s important to empower people to look after their own patients. A job well done is ultimately making yourself redundant.”
Training anaesthetists in war zones
“I first heard of the Foundation after reading War Doctor. As a fellow humanitarian, I could relate to David’s experiences. When I heard the Foundation wanted to develop an anaesthetics training module, it felt like a great fit for me.”
In October, Elma, David and a small team of trainers travelled to Poltava and Zhytomyr to deliver two HEST courses – Elma’s first time in Ukraine since the war began.
The team flew to Warsaw and with the support of our partner, UOSSM International, crossed the border before driving for most of the day to eastern Ukraine.
“During our first course in Poltava, there was a lot of unknown. We designed the module ourselves but didn’t know exactly who we’d be training or how it would be received.
In the end, we trained around 10 anaesthetists in Poltava and 12 in Zhytomyr and it was wonderful – I think they found it refreshing to have dedicated trauma training with practical advice. They were really excited to handle different kit and learn new techniques.”
Adapting in conflict
When it comes to war anaesthetics, there are two main considerations. Firstly, the injuries anaesthetists face in war are starkly different to cases seen in the west.
“Blast injuries from explosives are devastating to the body. Patients can have multiple life-threatening injuries and lose so much blood. The priority is stabilising the situation and giving blood.
We taught specific techniques for giving drugs and blood via the bone (intra-osseous), for when you can’t find a blood vessel. Many had not used this life-saving equipment and really benefited from learning this skill.
Many of these cases would need care on the intensive care unit – supporting patients with complicated head and lung injuries on our breathing machines and giving dialysis therapy to people with kidney failure as a result of crushing injuries.”
The other consideration in a war setting is reduced resources. Hospitals may be faced with electricity cuts or low oxygen supplies.
“We trained the groups on alternative anaesthesia machines – very different to ones we use in our hospitals here. They are portable enough to fit into a bag or small case and they can be life-saving in critical conditions – when you don’t have electricity or oxygen yet need to perform emergency operations.”
Teaching the group how to use basic machinery, available in most hospitals, will help them continue to save lives despite slashed resources.
“The rest of the world hasn’t forgotten you”
“Often, I think when you are stuck and living within conflicts, you feel the rest of the world has forgotten you.
But seeing people travel far distances to come and help, standing in solidarity with them, I hope shows them some humanity.”
Contemplation on safe ground
“It can be challenging dealing with the trauma of what you experience on missions. Often its worse when you get back home and have time to process things, devastating things you’ve seen.
The more missions I’ve done, the more I realise the importance of looking after yourself. Finding time to have breaks, even on busy missions. In Yemen, we were working and living in the hospital. Each day around 5pm I would try and go to the roof for 10 minutes to take in some fresh air, watch the sunset, whilst listening to the atmospheric call for prayer from the nearby mosques. It was time just for me.
The important thing is to be kind to yourself – and ask for help when you need it.
When reflecting on my time in Ukraine, it’s difficult to know quite how to describe how I feel. ‘Privileged’ comes to mind – for being able to work hand in hand with people on the ground and support them as best I can.”
- Surgical trainings in Ukraine - 1st May 2025
- Ukraine: the significant challenges of the present and what the next decade will hold - 13th February 2025
- Funding a Palestinian doctor for paediatric trauma training - 3rd February 2025