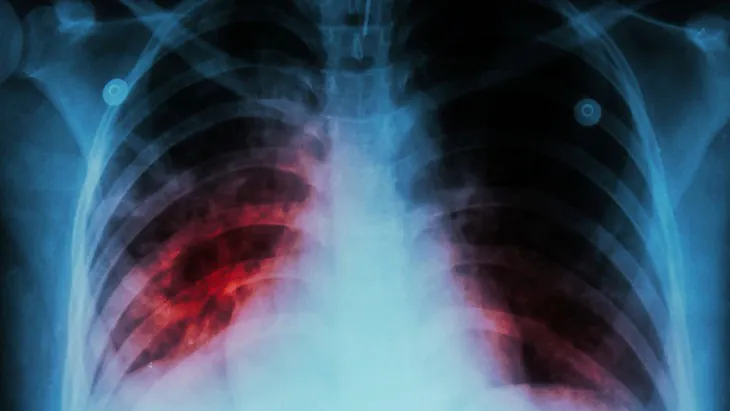
TB is an airborne infectious disease caused by Mycobacterium tuberculosis which most commonly affects the lungs. However, TB can also be ingested orally, and this may be the mode of transmission among people who eat raw milk products – often in other countries – before settling in the UK.
It is still a rare to see ingested TB but doctors need to be aware of the symptoms since the outcome of untreated ingested TB can be serious, particularly for children with less developed immune systems.
Patients may often only come to a doctor when their symptoms are already severe. In around two per cent of cases, the bacteria can lead to meningitis and peritonitis is another recognised complication. Typically, patients with ingested TB will report many months of suffering gastric upsets and tenderness in the gut. When the bacteria is consumed, it makes its way to the intestines and is taken up by the lymph nodes in the ileum. From there, it produces symptoms that can be confused with appendicitis.
In some people, the process will stop there and the TB bacteria are engulfed by white blood cells and trapped inside a spot of calcification. This process can also occur when the airborne bacteria attacks the lungs. The bacteria is not necessarily killed but it is immobilised, at least for the present.
In others, the bacteria prove too overwhelming and make their way into the bloodstream where they can cause a range of illnesses including high fever, septicaemia and TB meningitis.
A five-year-old child with TB meningitis may be unresponsive and clinicians may not immediately realise that TB is the pathogen, treating instead with penicillin which will have no effect on the Mycobacterium turbeculosis. Only a cerebral spinal fluid tap will show up the cause and this can take some hours.
Anti-TB drugs including streptomycin should be effective in most cases and should be used as soon as possible. Sadly, between 15-30 per cent of patients will die, despite receiving treatment and care.
- Patient case studies - April 21, 2016
- Signs of ingested TB - March 23, 2016
- A ground-breaking elective in the Yemen – over 50 years ago. - March 13, 2016