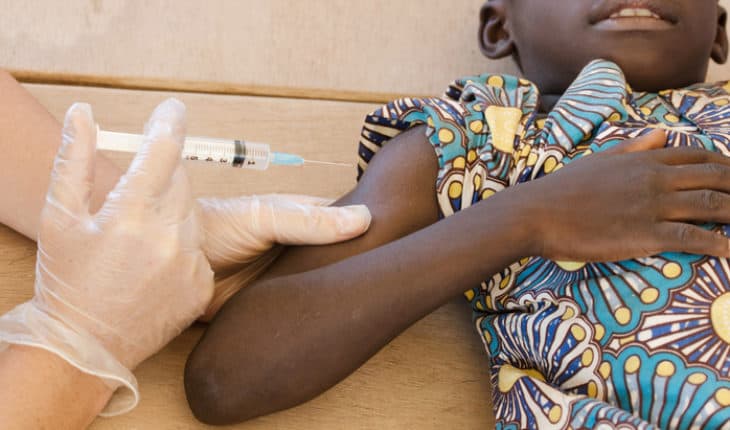
African kids among those to miss medical appointments due to COVID: Patients seeking treatment for HIV, malaria, tuberculosis, maternal and child health services missed vital appointments because of the pressures COVID-19 put on Africa’s health systems, new research has found.
The research, published today in BMJ Global Health, found examples of up to half of South African children not attending child health checks, as many as 80 per cent of children in Sierra Leone aged under five years not receiving routine vaccinations, more than half of Rwandan HIV patients missing antiretroviral treatments, and sex workers from Kenya being unable to access contraception or medical appointments.
Lead researcher Dr Gizachew Tessema, from Curtin University’s School of Population Health, said almost all African health systems had been impacted severely by the pressures of COVID, despite the late start and slow progression of the pandemic across the continent.
“Following the pandemic, our study showed the flow of patients accessing general and essential health services such as HIV care, treatment for malaria and tuberculosis, maternal and child health services has significantly reduced,” Dr Tessema said.
“Many patients reported missing scheduled medical appointments for chronic illnesses including HIV care and treatment. Africa’s health systems were ill-prepared for the COVID-19 pandemic as all available resources, including human, financial and material, were inadequate.”
Dr Tessema, an NHMRC Emerging Leadership Fellow, said the impact of the pandemic on Africa’s health systems served as a wake-up call, highlighting the urgent need for a coordinated response.
“The COVID-19 pandemic is not the first pandemic to hit Africa, nor will it be the last. The African health systems will continue to be confronted by emerging global and local events, including conflict, a potential new infectious disease, climate change, and the increasing burden of non-communicable diseases,” Dr Tessema said.
“Countries should direct their efforts to building a resilient health system that caters to all health challenges, times, and people. This requires local, national, and global collaboration and engagement to increase healthcare funding in Africa.
“Now that the world has effective COVID-19 vaccines, African countries need to embark on a coordinated capacity-building effort focused on developing, transporting and rolling out vaccinations for healthcare professionals and high-risk individuals, including across rural areas.”
The full paper, titled ‘The COVID-19 pandemic and healthcare systems in Africa: A scoping review of preparedness, impact, and response’, can be viewed online here.
- New lipid-based pathway discovered as key to memory formation - 25th June 2025
- Crucial link could explain how Alzheimer’s takes hold - 25th June 2025
- Understanding Your Mind Can Improve Daily Life - 25th June 2025