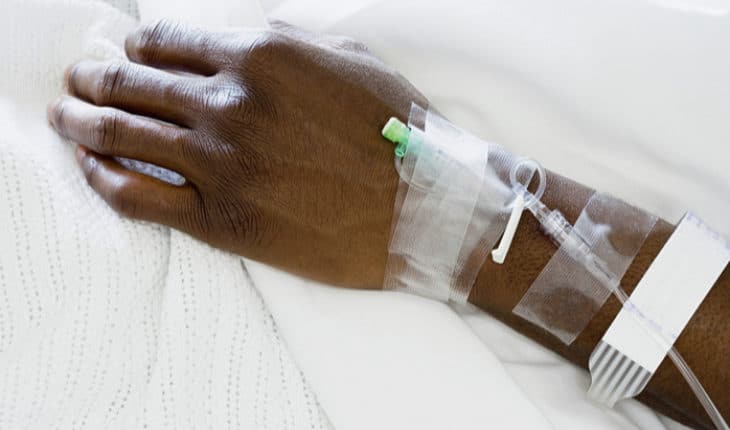
COVID-19 patients admitted from more deprived regions are at higher risk of intensive care admission, new study finds.
Black, Asian minority ethic patients with COVID-19 are more likely to be admitted to hospital from regions with higher levels of air pollution, lower quality housing and overcrowded living conditions and are more likely to be admitted to intensive care, a new UK study has found.
Led by Dr Marina Soltan at the University of Birmingham, the research analysed data from 408 hospitalised COVID-19 patients admitted to the Queen Elizabeth Hospital in Birmingham between 1st March and 13th April 2020. Patient postcodes were analysed according to their rating on the Index of Multiple Deprivation (IMDS), which takes into account the levels of crime, education, health and disability, income, employment, barriers to housing and services (BHS) and living environment (LE) of a particular area.
Data from the UK Office for National Statistics suggests that patients in the most deprived regions of the UK are twice as likely to die of COVID-19 than from other causes while the Intensive Care National Audit and Research Centre have reported that 34% of critically ill patients have come from BAME backgrounds, despite this group only accounting for 14% of the UK population. This latest study is the first of its kind to explore the roles of social determinants of health and their effect on the presentation of COVID-19 symptoms, ITU admissions and outcomes among patients of all ethnicities.
Researchers found that high air pollution and lower housing quality were potential risk factors for patients presenting to hospital with multi-lobar pneumonia and, in turn, being admitted to an intensive care unit, while patients admitted from overcrowded households were more likely to be admitted to an intensive care unit. Male patients were more likely to be hospitalised than female patients, while patients from areas with the highest barriers to housing and services accounted for 47.4% of all admissions.
Importantly the study found that patients of BAME ethnicity were more likely than white patients to be admitted from regions with high levels of air pollution, lower quality housing or overcrowded living conditions. 69.9% of BAME patients included in the study were populated within areas of high living environment deprivation compared to 50.2% of White patients. It is thought that this could begin to explain the higher levels of intensive care admissions amongst this group. Patients of BAME ethnicity were also younger than White patients – on average 61.85 years old compared to 69.5 for White patients.
Interestingly, irrespective of household overcrowding deprivation, air pollution deprivation and household quality deprivation, existing health conditions including ischaemic heart disease, chronic kidney disease, dementia and hypertension increase the risk of death among COVID19 positive patients across all ethnicities.
Lead author Dr Marina Soltan from the University of Birmingham said: “Our findings have potential public health implications and implications for how we develop clinical risk management tools including how we train clinicians to undertake the most important aspect of a clinical consultation effectively – history taking. The findings are also significant in understanding more about the effects of overcrowding and air pollution in BAME households not just in the UK but internationally.
“The next steps for this research are to take what we have learned in Birmingham and apply to that to other areas of the country; we are currently leading a multi-centre study working with other centres nationally to gain a wider understanding across multiple geographical locations.”
- New lipid-based pathway discovered as key to memory formation - 25th June 2025
- Crucial link could explain how Alzheimer’s takes hold - 25th June 2025
- Understanding Your Mind Can Improve Daily Life - 25th June 2025