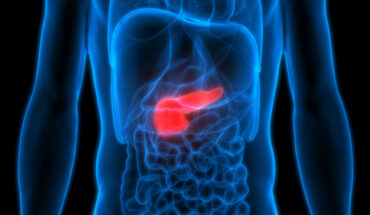
Magic rays that cure all cancers or expensive vanity projects of no real clinical value? That has been the argument up to now when it comes to proton beam therapy for cancer. However, I believe the argument is pretty much won now, not least because Aysha King, 6, who underwent proton beam therapy in Prague – landing his parents in jail because they stopped his treatment in the UK – is apparently cancer-free.
But one case study on its own is not enough to sway the doubters. Fortunately, even more convincingly, a recent paper in Lancet oncology (30th January 2016) from Boston showed considerable reduction in normal tissue damage in a large number of children treated with protons for a rare type of brain tumour. This careful study was very encouraging for the proton community as a whole because it justifies all the other studies in other more common cancers currently in progress. Over the next two years I believe there will be good evidence emerging that around 10 per cent of patients receiving radical radiotherapy would do better with protons. This would need 18 machines for the UK and without good forward planning will push Britain back in the quality tables of radiotherapy unless action is taken now.
The discovery of X-rays and gamma rays in late 19th century led to a revolution in diagnosis and treatment of cancer. In 1903 William Bragg, a British physicist discovered the very surprising behaviour of proton radiation. Protons are sub-atomic positively charged particles now
produced by accelerating protons in a circular accelerator called a cyclotron. The advantage of protons lies in something called the Bragg Peak. This is the key to understanding why protons may be better for some patients.
The aim of radiotherapy is to deliver as high a dose as possible to the cancer but to spare as much as possible critically sensitive normal tissues around it. Certain organs are particularly sensitive – the spinal cord, base of brain, eye, intestine, liver and kidneys. The Bragg peak allows a more precise conforming of high dose to the cancer sparing any tissues downstream of the beam.
Before they reach the cancer, both proton and conventional radiation types have to make their way through the patient’s skin and surrounding tissues. The photon, with no mass or charge, is highly penetrating and delivers a dose throughout any volume of tissue irradiated. However, most of the radiation is delivered only half a centimetre from the patient’s skin, depending on the energy it was initially given. It then gradually loses this energy until it reaches the target. As tumours are almost always deeply located in the body, the photon actively interacts with outer healthy cells and drops only a small remaining dose of ionizing radiation on the deeper diseased cells. Moreover, as photons are not all stopped by human tissue, they leave the patient’s body and continue to emit radiation as they leave the body. This is called the exit dose.
The proton, on the other hand, is a heavy, positively charged particle that gradually loses its speed as it interacts with human tissue. It is easily controlled and delivers its maximum dose at a precise depth, which is determined by the amount of energy it was given to it by the cyclotron. The proton is very fast when it enters the patient’s body and deposits only a small dose on its way. The absorbed dose increases very gradually with greater depth and lower speed, suddenly rising to a burst when the proton is ultimately stopped. This is the Bragg peak. The behaviour of the proton can be precisely determined and the beam can be directed so the Bragg peak occurs exactly within the confines of the cancer. Immediately after this burst of energy, the proton stops completely – its energy all spent. Proton therapy therefore allows to target cancers deep inside the body more precisely and spares critical surrounding tissue. The problem is cost. Protons are nearly 2,000 times as big as electrons. Accelerating electrons down a long, straight tube is how conventional linear accelerator (LINAC) based radiation is produced. But protons require far more energy to get them moving. So a cyclotron is used accelerating them round and round in circles getting faster and faster. These are large and expensive bits of kit costing up to £100m with another £25m for the building to house them. Recently costs have fallen and a compact model can be bought for a cool £25m. This compares with £2.5m for a conventional radiotherapy machine.
So what are the cost implications?
Proton beam therapy is currently horrendously more expensive than conventional LINAC based radiotherapy. With legacy systems the cost ratio of protons/conventional is nearly tenfold. With compact systems and adequate numbers of patients this falls to below two. As the price differential diminishes, it is likely that there will be increasing demand of protons where the planned target volume can be achieved with greater critical normal tissue sparing by using protons.
It is now unlikely that there will ever be large scale randomised clinical trials but rather a pre-treatment comparison of proton versus conventional radiotherapy in individual patients using predetermined metrics of plan quality. This assessment would be made objectively by treatment planning software system. Payers, both governments (such as the British NHS) and insurers will use these criteria to assess the value of proton to an individual patient using the equation:
VALUE = QUALITY + ACCESS/ COST OF TREATMENT
This formula applies to any service whether it’s a cup of coffee from a café or a complex cancer treatment. Such analyses will determine the level of the therapeutic plateau in the relationship of cost to clinical outcome gain.
Unfortunately, a literature review can only be of limited value in predicting demand for protons and how market forces will interact with evidence based studies in the minds of payers. Furthermore, technology shifts with a steady increase in the quality of imaging, planning and delivery of both protons and conventional radiation makes studies carried out even three years ago less relevant.
The use of protons is likely to be indicated for three groups of patients.
1. Hard indications – mainly children with spinal cord and brain tumours
2. Cancer types where a significant proportion of patients are likely to benefit – lung and prostate through reduced long term side effects
3. Patients where the anatomy of the tumour and critical normal tissues favours a dose distribution with protons. This could be of any cancer type or site where radical radiotherapy is being proposed. That means the radiation is being given with the aim of eradicating the cancer so curing the patient.
Calculating the demand for protons and the number of machines needed for a given population is difficult. The literature is weak, consisting mainly of calculations based on committee opinions of likely future indications and dovetailing this with past epidemiology from cancer registries. There are six such studies identified. There are no randomised controlled trials and these are unlikely in the future. A major problem in any analysis is the gradual improvement the dose distribution achievable by conventional linear accelerator delivered radiation over the last decade. Comparisons to conformal therapy are not so relevant in an era of IMRT, VMAT, SABR and 100 per cent IGRT. These acronyms are the new buzzwords of the radiotherapist and allow for much greater accuracy in radiation delivery.
The most informative study was carried out in Boston, USA. Here a comparison was made of proton versus conventional plans retrospectively in all patients treated over a one-year period in 2008. 1042 patient plans were analysed and scored. This allows the potential proton utilisation scenarios as a percentage of total fractions delivered to be calculated. The two main weaknesses of this study are the use of conformal therapy and not IMRT as a comparator and the optimistic committee judgement in an academic US centre to assess percentage of proton utilisation. They concluded that 17 per cent of all patients would have benefited from the use of protons.
Several proton demand studies have been carried out. Not surprisingly the results differ between countries with the USA at 20 per cent, Sweden 16 per cent, Italy 13 per cent, France 12 per cent, Holland and the UK 10 per cent.
Let’s look at what this would mean for the UK. The estimated demand for proton machines is based on a capacity per unit of 500 patients annually (20 average fraction delivery time, 25 fractions per course, 12 hour working 6 days per week). At a 10 per cent level the machine requirement for the UK is therefore 18 machines. If an 18 hour double shift working day is implemented treating 750 patients annually then the requirement could be reduced to 12 machines.
Is this achievable? So far two machines very slowly being installed one at University College Hospital in London and the other at Christie Hospital, Manchester. The money was allocated in early 2011 and there has been more talk than action. Large legacy machines have been chosen costing £80m and requiring 80 staff each to run them. The compact models being installed by private sector providers but for NHS use cost less than £25m and require only 20 staff. That means the cost per single treatment will be far more
expensive in the NHS installations. If everything is taken into account the UCLH/Christie true cost per treatment will approach £5,000 whereas the compact model cost will be less than £1,500. And remember that most patients will need at least 20 treatments every day for four weeks.
We know that the average quality of British radiotherapy is poor with a huge need to upgrade the routine delivery machines many of which are more than a decade old. Capital is short as the NHS heads for a £20bn deficit by 2020. Imaginative new ways of funding state of the art cancer care are urgently needed in the UK and in many other countries. The disease is rapidly rising in incidence as populations get older and we really need to improve the care we give to all our patients.
Declaration of interest: Karol Sikora is currently medical adviser to Proton Partners International a private equity backed venture building three proton beam centres in the UK in Newport (South Wales), Northumbria and West London.
- Cancer backlog will become a national emergency - 4th June 2020
- Cancer –a story that concerns every one of us - 20th June 2017
- Restrictive diets - 15th May 2016