Vascular disease in COVID-19 is not caused by viral infection of blood vessels: The SARS-CoV-2 virus does not infect blood vessels, despite the high risk of blood clots to COVID-19 patients, University of Queensland researchers have found.
Dr Emma Gordon and Dr Larisa Labzin from UQ’s Institute for Molecular Bioscience and Dr Kirsty Short from UQ’s School of Chemistry and Molecular Biosciences pooled their expertise in vascular biology and virology to determine how the virus causes damage to blood vessels.
The researchers found that the cardiovascular complications of COVID-19 are triggered by inflammation caused by infected airway cells.
“At least 40 per cent of patients that are hospitalised with COVID-19 are at high risk of blood clots, and anti-coagulation therapies are now being routinely used,” Dr Gordon said.
“There have been many studies attempting to prove whether the virus is infecting cells of the inner blood vessel wall or not.
“By conducting our experiments using real, infectious virus rather than fragments of the virus’s spike protein, we can definitively say it is not.”
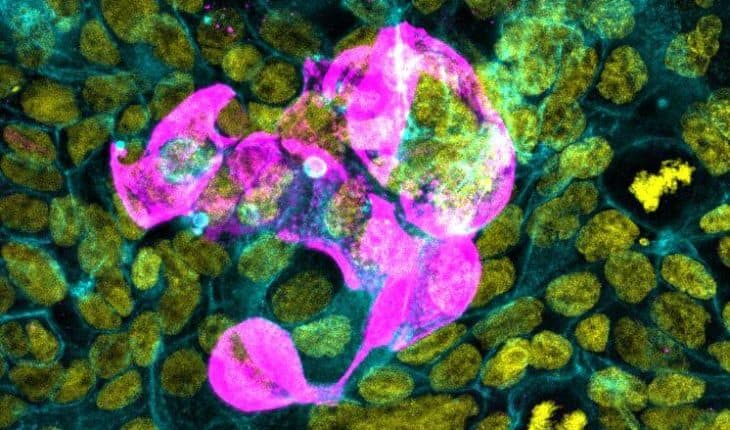
The researchers used UQ’s sophisticated microscopy facilities to track where the virus travelled in the cells and visualise how blood vessels respond to the live virus.
Immunologist Dr Labzin said the body’s inflammatory response had a big effect on the cardiovascular system because they work together to fight infection – the blood delivers the immune cells to the site of infection and makes blood clots if the blood vessel is damaged.
“When our immune system works well, it clears the virus from our bodies,” Dr Labzin said.
“But sometimes it goes into overdrive and we get an overblown inflammatory response causing complications –in the case of COVID-19, this is often blood clots, when there shouldn’t be any.
“Knowing that it is inflammation causing these cardiovascular complications arising from COVID-19 rather than the virus itself will help us develop the right treatments, and a better understanding of how and why these complications arise.”
Heart Foundation interim CEO, Professor Garry Jennings said the study helps clarify a key debate about the relationship between the virus and the lining of the blood vessels.
“How the cells lining the blood vessels sense the virus and the damage to nearby cells is still not completely understood,” he said.
“There is more research to do, but this study is an important step in our understanding of the virus and which cells and mechanisms we should look at next.”
This research is published in Clinical and translational Immunology (http://doi.org/10.1002/cti2.1350).
This work was supported by a Future Leader Fellowship (104692) from the National Heart Foundation of Australia and the National Health and Medical Research Council.
- New lipid-based pathway discovered as key to memory formation - 25th June 2025
- Crucial link could explain how Alzheimer’s takes hold - 25th June 2025
- Understanding Your Mind Can Improve Daily Life - 25th June 2025