At the start of my internship, a 16-year-old girl was brought into the emergency room; she was in a coma.
She had been sick for a long time, and her family abandoned her as they thought she was pregnant. It was her neighbour who brought her to the hospital.
The girl was very skinny for her age. She was very weak, and she had been very thirsty and going to the bathroom frequently.
After laboratory tests, we diagnosed her with type 1 diabetes. Because of her illness, she had dropped out of school.
According to the 2015 International Diabetes Federation Atlas (IDF), 5 million people die because of the complications diabetes, and oftentimes, because they ignored the fact that they had such a disease. In 2014, the IDF estimated that 193 million people unknowingly have diabetes, just like the girl in the emergency room. In most cases, they have type 2 diabetes.
Diabetes is the 3rd major cause of hospitalization in Burundi’s biggest hospital after malaria and HIV.
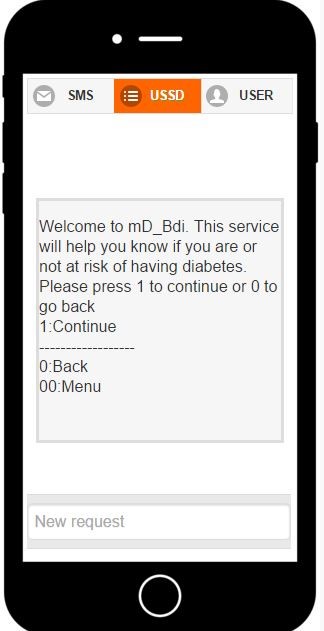
Given the recent rise in mobile penetration rates in Africa, mobile technologies and applications can provide a unique platform for increased rates of screening. In Burundi alone, the rates of mobile subscribers have skyrocketed from 0 in 1999 to 2.5 million out of a population of 10 million in 2012.
There are several complications associated with diabetes including chronic kidney disease, heart failure, retinopathy (blindness), and neuropathy. Others include diabetic ketoacidosis (coma), or hypoglycemia (glucose deficiency) which requires insulin treatment.
When a person has been living undiagnosed with diabetes for a long time, the opportunities and potential benefits associated with a proper diagnostic are lost.
The cost associated with undiagnosed diabetics is considerable. The overall increased use of health services, loss of productivity, and the disabilities the illness poses can be a heavy burden for the individual, their family, and society. In a country like Burundi, where 65 per cent of the population earns less than $1.25 a day, not many people can afford dialysis for kidney failure, which costs about $31,200 a year. Only a tiny portion of the population has health insurance.
It is clear that early diagnosis is imperative in order to treat the disease in time and thus prevent serious and expensive complications. Unfortunately, no African country has diagnosed all of these cases of diabetes. In sub-Saharan Africa, where medical resources are often lacking and testing for diabetes isn’t always a priority for governments, the proportion of undiagnosed people reaches 90 per cent in countries like Burundi.
As a solution, Burundi 3.0’s project, “mDiab Burundi”, provides the screening of risk factors associated with diabetes as well as educating the population about the disease using mobile technology.
In 2013, Burundi 3.0 initiated a project to send SMS alerts to job opportunities for young job seekers. Since then, 15 000 people have signed up to the job alerts, and they have reported the solution to be cheaper than advertisements in newspapers.
Last year, we received funding from the Tony Elumelu Foundation through their Entrepreneurship Program which has helped us further develop our mobile applications. Burundi 3.0 has also been invited to the Clinton Global Initiative Middle East and Africa and the Global Entrepreneurship Summit in Silicon Valley.
Through further development of mobile applications, there is an opportunity to reach a significant portion of the population that cannot ordinarily gain access to health facilities for screening of risk factors associated with type 2 diabetes.
Mobile technology has done miracles in other sectors as well, like mobile banking throughout Africa. Why not do the same things in the field of medicine and healthcare?