New epilepsy research reveals brain wiring differences: Children with epilepsy have brains that are wired differently from those without the condition, a new study by our researchers has found. This new epilepsy research paves the way for improved treatment, specifically how different surgery techniques can treat children and young people with epilepsy.
A collaborative project, the research team comprised researchers from Great Ormond Street Hospital (GOSH), UCL Great Ormond Street Institute of Child Health (UCL GOS ICH), King’s College London, The University of Pennsylvania, and Nemours Children’s Hospital, underpinned by support from GOSH National Institute of Health Research Biomedical Research Centre.
How epilepsy affects a child’s brain
The research team used a technique called diffusion MRI to analyse wiring diagrams of the brain, enabling them to see how strongly different areas of the brain are connected. Using this diffusion MRI technique, they were able to understand how:
- the children with epilepsy had differently wired brains; they had more connections than children without epilepsy
- these unusual wiring dynamics could make children with epilepsy more likely to have epileptic seizures
- the children whose seizures stemmed from multiple areas of the brain had greater differences in wiring than those with seizures stemming from only one area.
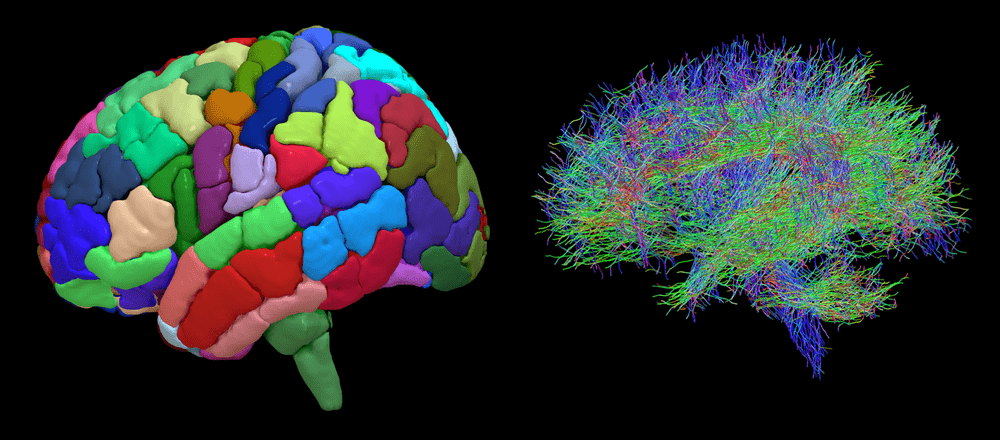
Structural imaging of the brain’s regions (left) and diffusion diagram of the wiring of a brain (right), which the team analyse together to create a ’network’ which helps them understand how a child’s brain works. Credit Aswin Chari
New findings to influence future epilepsy treatment
Of the 79 children with epilepsy who were part of the study, 52 had surgery to remove the brain regions responsible for their seizures.
The researchers found that the brain areas removed had particularly more abnormal wiring than other brain regions. By removing them, they were able to create more normal wiring dynamics in the brain.
Whilst not all of the children who took part in this study were cured of their seizures, the research team hopes that the technology and analysis used in this research will pave the way for further studies – leading to improved surgical outcomes and more children being offered the procedure.
Read more about this research in the medical journal, Communications Biology.
Aswin Chari, the Lewis-Spitz Surgical Scientist, led the team carrying out this epilepsy research. GOSH Charity funds Mr. Chari’s role and research.
“I am delighted to share the findings of this study, in which we used diffusion MRI technology to teach us about the function of children’s brains, helping to deepen our understanding of debilitating conditions like epilepsy.
“Although surgery for epilepsy is relatively safe, it is a large undertaking and there are some children who undergo surgery but sadly continue to have seizures.”
We hope through this technology and analysis, we can enable more children with the condition to benefit from life-changing surgery and treatment.
Aswin Chari, the Lewis-Spitz Surgical Scientist, at Great Ormond Street Hospital, funded by GOSH Charity.
A collaborative approach to epilepsy research
Great Ormond Street Hospital (GOSH), UCL Great Ormond Street Institute of Child Health (UCL GOS ICH), King’s College London, The University of Pennsylvania, and Nemours Children’s Hospital, worked together to understand more about epilepsy in children. Our GOSH National Institute of Health Research Biomedical Research Centre’s support underpinned this research study.
It comes almost a year after the Royal College of Paediatrics and Child Health (RCPCH) published their Epilepsy 12 report, highlighting:
- three quarters (77%) of children who should have been considered for epilepsy surgery in November 2020 had not been referred.
- issues around waiting times for tests, treatment, and referrals to paediatric neurologists.
While these figures can be partly attributed to the COVID-19 pandemic’s impact on healthcare, Mr. Chari and his team hope their findings will mean more children can be diagnosed and treated more effectively and efficiently.
- New lipid-based pathway discovered as key to memory formation - 25th June 2025
- Crucial link could explain how Alzheimer’s takes hold - 25th June 2025
- Understanding Your Mind Can Improve Daily Life - 25th June 2025