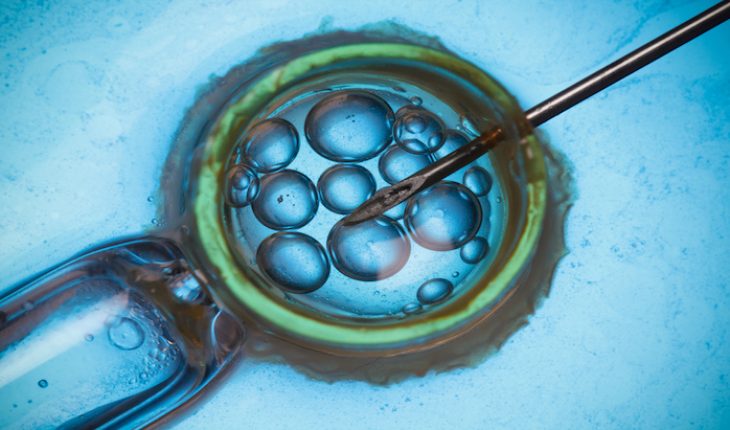
Snowflakes have been described as ‘tiny miracles of beauty’. Wilson Alwyn “Snowflake” Bentley photographed more than 5000 in his lifetime, showing their intricate, individual form. Inspired by their uniqueness and fragility, “Snowflake Embryo Adoption” was established in America in 1997. To date, 479 babies from frozen embryos have been born to adoptive families through this organisation, which has been endorsed by George Bush and continued to receive funding from President Obama.
My husband and I adopted embryos in the UK in 2008. The treatment failed and, as well as empty arms, the Blood Transfusion Service suggest that I may be stained much deeper within.
The Surplus of Snowflakes
Snowflake embryos are frozen embryos left over after IVF treatment. Some reports estimate that 600,000 embryos lie suspended in ice in the United States today. Statistics for England are not made public, but with a round of IVF sometimes creating 18 embryos, and 47,422 women undergoing IVF in the UK in 2012, a lot of embryos will remain unused. One statistic suggests that 2 million embryos remain frozen globally, with more added daily.
The question as to what to do with the surplus embryos weighs on many parent’s minds (see the recent article in the Guardian entitled “Should I defrost my freezer boys?”) Parents can choose to keep them frozen, destroy them or donate them to science.
We chose to adopt embryos as a way to have children. The procedure was relatively inexpensive, the hormone treatment simple (a nasal spray to prepare the womb), and we did have long discussions about the ethics and questions inevitably raised. The treatment failed, but we had been warned that, unsurprisingly, embryos were not designed to be frozen. Every time I witness a snowflake melt or sublime, I remember the perished embryos, too fragile to sustain life after being frozen.
The Stain
Childlessness can be hard. We will miss out on the milestones that parents anticipate: their first word, their first day at school, their exam results, their first date, their leaving home, the arrival of grandchildren. Well-meaning friends ask whether we might adopt or try fertility treatment.
I accepted our condition and resumed normal activities, one of which was to be a blood donor. I had already donated 10 units, and was aiming to emulate my biology school teacher who had given well over 50 units. I had seen the desperate need for blood during my time as a nurse. I am still haunted by the thought of one particular man, dying of liver failure, drowning in melaena. Bags of blood were pumped into him as fast as they poured out. Soon a senior doctor declared an end to the transfusion: the patient was too sick and the blood was in short supply.
My blood, however, would not be able to help patients like these. The Blood Transfusion Service does not accept blood from women who have received donated eggs or embryos on the ground that a woman who died from new variant Creutzfeldt Jakob disease (vCJD) in another country was found to have the prions in her ovaries.
This information left me reeling. Was I diseased? I hadn’t received a baby, but had I been contaminated? Why had I not been informed of this risk during the consent process? As an identical twin, with a sister who once had critically low levels of white blood cells, I had always prided myself on being able to donate to her. What if she needed a donation in the future? Would I no longer be her lifeline?
The Stain Deepens
The exclusion zone reaches beyond those of us who have received eggs or embryos. For over 50 years, the urine of postmenopausal women has been used in fertility treatments (not many people know this). Their urine contains high levels of gonadotrophins, able to stimulate egg and sperm production in couples facing infertility. One such drug, Metrodin, renders its recipients unable to donate blood because the country in which it was produced (Italy) had a case of variant CJD.
Many women don’t know or can’t remember the fertility drugs that they were treated with. In an absurd twist, such women can still donate blood. Forgetfulness, it appears, acts as an efficient stain remover.
The British Fertility Society do not believe that such drugs or products carry any risk of contamination, yet the stain remains on hundreds of women as guidance from the Medicines and Healthcare products Regulatory Agency (MHRA) dictates that our blood should be blacklisted.
The Shortage of Blood Donors
Last week I anonymously called my local blood donation centre and was welcomed as a potential new donor until I revealed my fertility treatment. The nurse was sympathetic and offered her apologies.
Last week my local newspaper also ran a story urging people to donate blood, noting that only four percent of the population give blood and numbers are falling.
NHS Blood and Transplant has launched its global Missing Type campaign, highlighting the decline in the number of people becoming donors. Could I be part of the missing link?
- Care Home Nursing: The World’s Largest Relay Race? - 13th August 2019
- Mouth Care Matters in Older People - 25th June 2019
- Dealing with illness in dreadful hot weather - 26th July 2018