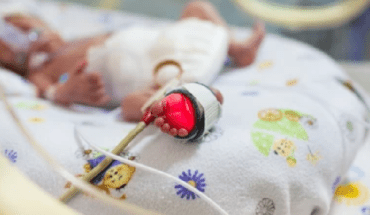
A year on from the first lockdown and after warnings from the mental health sector about the impact of the pandemic on the country’s mental health, NHS Digital data shows that while the crisis is affecting people of all ages, it is under-18s who are suffering most.
The Royal College of Psychiatrists’ analysis found that:
- 80,226 more children and young people were referred to CYP mental health services between April and December last year, up by 28% on 2019, to 372,438.
- 600,628 more treatment sessions were given to children and young people, up by a fifth on 2019 to 3.58 million.
- 18,268 children and young people needed urgent or emergency crisis care – including assessments to see if someone needs to be sectioned because they or others are at harm – an increase of 18% on 2019, to 18,269.
The Royal College of Psychiatrists is calling for the additional £500 million in the Government’s mental health recovery plan to urgently reach the frontline so that people can get the support they need. This funding is on top of the existing planned investment in mental health services set out in the NHS Long Term Plan.
Dr Bernadka Dubicka, chair of the child and adolescent faculty at the Royal College of Psychiatrists, said: “Our children and young people are bearing the brunt of the mental health crisis caused by the pandemic and are at risk of lifelong mental illness.
“As a frontline psychiatrist I’ve seen the devastating effect that school closures, disrupted friendships and the uncertainty caused by the pandemic have had on the mental health of our children and young people.
“Services were already struggling to cope with the number of children needing help before the pandemic hit, and they risk being overrun unless government ensures the promised money reaches the frontline quickly.”
The crisis is affecting adults as well as children. Over one million more treatment sessions were given to adults between April and December last year (1,078,539), an increase of 8% on 2019. There was also 159,347 urgent or emergency crisis referrals made for adults, an all-time high, and an increase of 2% on 2019.
Dr Adrian James, president of the Royal College of Psychiatrists, said: “The extent of the mental health crisis is terrifying, but it will likely get a lot worse before it gets better.
“Services are at a very real risk of being overrun by the sheer volume of people needing help with their mental illness.
“While the recent funding announcement is welcome, we need this money to reach mental health services as soon as possible to tackle this crisis.”
More children than ever before are being treated by eating disorder services and waiting for the care they need. There have also been huge increases in the number of people reporting moderate to severe depressive symptoms, and the number of people reporting being lonely has reached record levels.
Sarah [not her real name], whose teenage daughter relapsed into anorexia during the pandemic, said: “The pandemic has been devastating for my daughter and for our family. She has anorexia and was discharged from an inpatient unit last year, but the disruption to her normal routines and socialising really affected her recovery. She was spending a lot less time doing the things she enjoys and a lot more time alone with her thoughts.
“Unfortunately, she relapsed, becoming so unwell she was admitted to hospital and sectioned. After 72 days in hospital with no specialist eating disorder bed becoming available, we brought her home where I am now tube-feeding her daily. My daughter urgently needs specialist help for this life-threatening illness, but because of increased demand services are completely overwhelmed. It’s a terrifying situation to be in.”
- New lipid-based pathway discovered as key to memory formation - 25th June 2025
- Crucial link could explain how Alzheimer’s takes hold - 25th June 2025
- Understanding Your Mind Can Improve Daily Life - 25th June 2025